Sacroiliac Joint Pain Relief Techniques That Don’t Involve Surgery
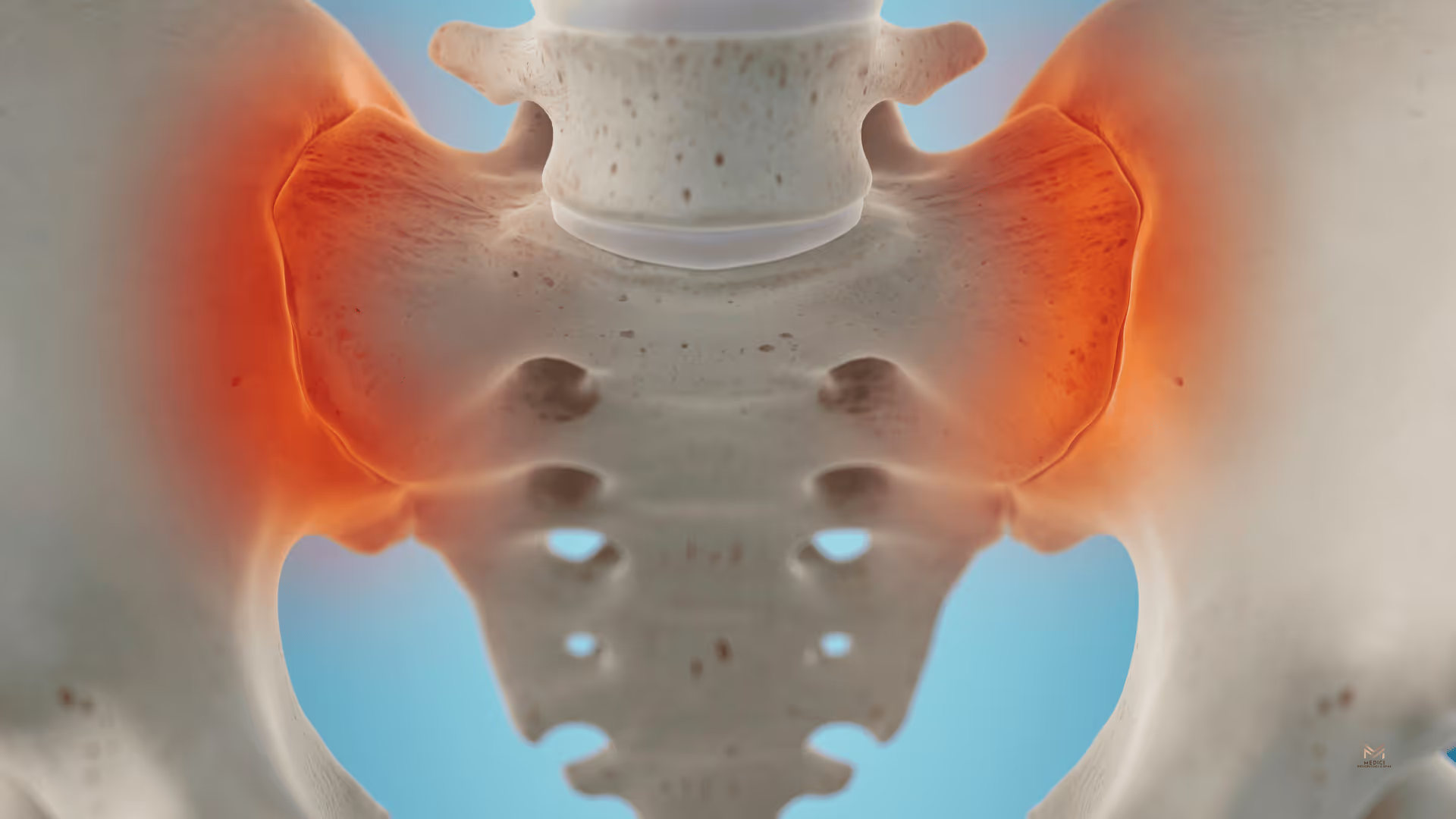
Sacroiliac (SI) joint pain can be surprisingly disruptive—and often confusing. It may affect how you walk, how long you can stand, how comfortably you can sit, and even how well you sleep. For many people, it’s not just “back pain.” It’s the kind of pain that shows up during simple transitions—getting out of a chair, climbing stairs, rolling over in bed, or stepping out of a car—and it can make everyday life feel unpredictable.
One of the most frustrating parts is that SI joint pain is commonly mistaken for low back pain or even sciatica. That mislabeling can lead to generic advice (“just stretch more,” “rest a few days,” “strengthen your core”) that doesn’t actually address the real driver. When the wrong structure is being treated, symptoms can linger—and patients understandably start to wonder if they’re stuck with it.
The good news is that many people find meaningful relief without surgery. A stepwise approach—one that restores pelvic stability, improves mechanics, and reduces inflammation—can calm symptoms and help prevent flare-ups from coming back. At Medici Orthopaedics & Spine, we focus on minimally invasive, drug-sparing, evidence-based care designed to restore quality of life and help you move confidently again.
Targeted Physical Therapy
Why PT Works for SI Joint Pain
Targeted physical therapy is one of the most effective non-surgical strategies for SI joint pain because it focuses on what the SI joint needs most: stable support.
It helps by:
- Improving pelvic stability so the joint isn’t repeatedly stressed with everyday movement
- Reducing compensation patterns (like overusing the low back or tightening the hip flexors)
- Retraining movement mechanics so bending, lifting, walking, and standing don’t keep triggering flare-ups
Key Components of SI-Focused PT
A high-quality SI program is not random stretching—it’s structured and specific:
- Core stabilization: Deep core control (transverse abdominis, multifidus) to support the pelvis and spine without bracing or over-tensing.
- Glute strengthening: Especially glute med/max to control pelvic position and reduce shearing forces at the SI joint.
- Hip mobility with control: Restoring motion where it belongs (often hips) so the SI joint doesn’t compensate.
- Gait and posture correction: Small changes in walking mechanics, stance, and weight shifting can reduce daily irritation.
- Gradual load progression + activity modification: You shouldn’t have to “stop living” to heal. The goal is adjusting the load so your body can recover while you stay functional.
Who Benefits Most
Targeted SI-focused PT is especially helpful for:
- Mechanical SI joint pain (movement-related, load-sensitive pain patterns)
- Recurrent flare-ups triggered by lifting, prolonged sitting, or standing
- Postpartum SI instability, where ligament laxity and core/glute weakness often play a major role
Manual Therapy & Myofascial Release
Techniques That Commonly Help
- Myofascial release (low back, glutes, hip flexors): These areas commonly become tight and overactive, especially when the pelvis is trying to stabilize an irritated SI joint. Releasing restrictions can reduce the pulling forces on the joint.
- Trigger point therapy (piriformis and surrounding tissues): Trigger points in the piriformis, glute med/min, and deep hip rotators can mimic sciatica-like symptoms or intensify buttock pain.
- Joint mobilization (where appropriate): In select cases, gentle mobilization to nearby joints (like the hips or thoracic spine) can improve movement patterns so the SI joint doesn’t have to compensate.
- Assisted stretching: Guided stretching helps lengthen tight, guarded tissues safely—especially when pain makes it difficult to stretch effectively on your own.
Why It Helps
- Decreases muscle guarding: Less bracing means less compressive stress on the pelvis and low back.
- Improves tissue glide and hip motion: When hips move better, the pelvis and SI region stop doing “extra work.”
- Reduces stress placed on the SI joint: You’re not just loosening muscles—you’re improving the overall mechanics that repeatedly irritate the joint.
Non-Surgical Relief Technique #3: SI Joint Belts, Bracing & Ergonomics
SI Belt Support
When to use:
- During flared pain or high-activity days
- Postpartum instability (when ligaments are looser and pelvic control is rebuilding)
- Prolonged standing or walking if symptoms increase with time on your feet
Proper placement and fitting tips:
- An SI belt should sit low, wrapping around the pelvis—closer to the level of the hip bones—not high on the waist like a back brace.
- It should feel supportive, not constrictive. If it causes numbness, tingling, or discomfort, it’s likely too tight or positioned incorrectly.
Ergonomic Adjustments
Small daily changes can make a surprisingly big difference:
- Sitting posture and seat height: Aim for hips and knees near 90 degrees, feet supported, and avoid slumping that shifts pelvic load unevenly.
- Getting in/out of a car: Pivot your whole body together—avoid twisting the pelvis while one leg is still outside.
- Lifting mechanics and hip hinging: Bend from hips, keep the load close, and avoid twisting while lifting (twist your feet instead).
- Sleep positions: A pillow between the knees (side-sleeping) or under the knees (back-sleeping) can reduce pelvic torque and night pain. Some people benefit from light pelvic support positioning.
Heat, Cold & Recovery Habits
When Heat Helps
- Muscle spasm and stiffness: Heat relaxes tight muscles that clamp down around the pelvis.
- Morning tightness: A warm shower or heating pad before gentle movement often reduces that “locked up” feeling.
When Cold Helps
- Acute flare-ups: Cold can calm irritated tissues and reduce pain signals.
- Inflammation after activity: If symptoms spike after standing, walking, or lifting, cold can reduce the inflammatory response.
Recovery Habits That Reduce Flares
- Sleep optimization: Poor sleep increases pain sensitivity and slows tissue recovery. Even small improvements in routine and positioning matter.
- Stress reduction (nervous system down-regulation): Stress increases muscle tension and can amplify pain signals. Gentle breathing, walking, and relaxation practices help.
- Hydration and anti-inflammatory nutrition: Hydration supports tissue health, and anti-inflammatory eating patterns may help reduce the “background inflammation” that makes flares more frequent.
Minimally Invasive Options at Medici
Image-Guided SI Joint Injections
- Diagnostic confirmation and therapeutic relief: Injections can help confirm that the SI joint is truly the pain generator while also calming inflammation.
- What patients can realistically expect: Relief may be temporary, but it often creates a valuable window to progress rehab, strengthen stabilizers, and improve mechanics for longer-term results.
- Why image guidance matters: Accuracy is key—image-guided injections improve precision and safety, helping ensure medication reaches the intended target.
B. Radiofrequency Ablation (RFA) for SI Joint Pain
- When considered: If SI pain is confirmed and injection relief is significant but short-lived, RFA may be appropriate.
- How it works: RFA calms pain signaling from targeted nerves that transmit SI joint pain.
- Benefits: Longer relief windows for appropriate candidates, often allowing greater consistency with strengthening and conditioning.
C. Regenerative Medicine & Prolotherapy
- Supporting ligament/tendon stability around the SI joint: These treatments aim to strengthen supportive structures and improve stability—especially in mechanical instability patterns.
- Best for: Patients whose SI pain appears driven by looseness/laxity and recurrent flare patterns despite good rehab effort.
- Responsible presentation: Evidence varies by condition and individual profile. These therapies are best used with careful selection and integrated with PT—not as a one-step cure.
Comprehensive Pain Management Without Heavy Medications
At Medici, pain management is guided by medication stewardship—using the lowest-risk plan that supports function and recovery.
- Emphasis on function, rehab, and targeted interventions: The goal is to help you move better and stay better.
- Options to reduce reliance on opioids: When medication is needed, the plan is conservative and strategic, with a strong focus on nonopioid approaches and therapies that address the true pain driver.
Stability, Comfort, and Confidence Can Be Restored—Without Surgery
SI joint pain can feel stubborn—especially when it’s been mislabeled as generic “low back pain” or treated with approaches that don’t match the true source. But here’s the reassurance many people need to hear: SI joint pain is common, and it’s highly treatable. For most patients, meaningful relief does not require surgery.
The best outcomes come from a plan that’s both precise and practical—confirming the true pain generator and then building long-term stability through targeted rehab. When pelvic mechanics improve, supportive muscles activate correctly, and inflammation is reduced in a strategic way, flare-ups often become less frequent and far less intense. The goal isn’t just to feel better this week—it’s to move confidently again and stay that way.
If your SI joint pain has been limiting your work, sleep, walking, or quality of life, Medici Orthopaedics & Spine is here to help. Our team specializes in drug-sparing, minimally invasive, evidence-based care, combining targeted physical therapy strategies with advanced diagnostic and interventional options when appropriate—always with your long-term function in mind.
Contact Medici Orthopaedics & Spine
🌐 Website: https://www.mediciortho.com/
📞 Main Contact: +1-844-328-4624
Ambulatory Surgery Centers
• Marietta – 792 Church Street, Unit 101, Marietta, GA 30060 | (470) 795-8398
• Snellville – 2220 Wisteria Dr, Unit 100, Snellville, GA 30078 | (470) 795-8398
Clinics
• Kennesaw – 2911 George Busbee Parkway, Suite 50, Kennesaw, GA 30144 | (770) 545-6404
• Snellville – 2220 Wisteria Drive, Unit 101, Snellville, GA 30078 | (470) 645-9297
• Buckhead PM&R – 3200 Downwood Circle NW, Suite 520, Atlanta, GA 30327 | (770) 872-7549