Herniated Disc Relief in Kennesaw: From Diagnosis to Recovery
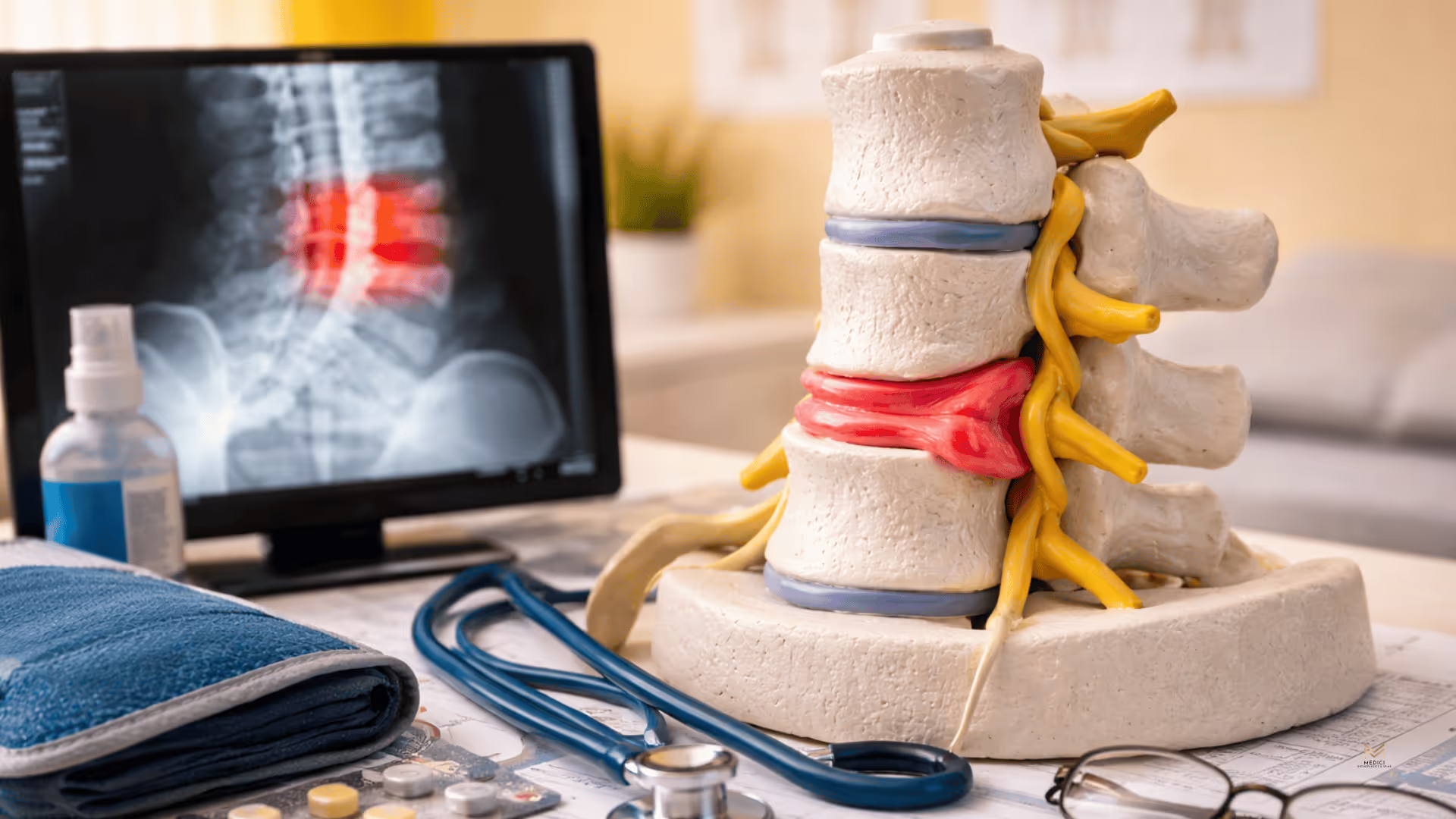
Living with back or neck pain can quietly take over your life. What starts as stiffness or soreness may progress into sharp, radiating pain that interferes with work, sleep, and even the simplest daily activities. For many patients in Kennesaw, this pain is caused by a herniated disc—an all-too-common spinal condition that is often misunderstood and, fortunately, very treatable.
A herniated disc develops when one of the spine’s cushioning discs becomes damaged and presses on nearby nerves. This can happen gradually over time or suddenly after an injury. The result may be persistent pain, numbness, tingling, or weakness that makes sitting, standing, or moving uncomfortable. Many people fear that a herniated disc automatically means surgery, but that is one of the biggest misconceptions we see. In reality, most patients improve with conservative, minimally invasive care—and effective options are available right here in Kennesaw.
With the right diagnosis and a personalized treatment plan, herniated disc pain does not have to define your life.
What Is a Herniated Disc?
Basic Spinal Anatomy Explained
Vertebrae
Vertebrae are the individual bones that stack on top of one another to form the spinal column. They provide structure and stability while creating space for the spinal cord and nerves to travel safely from the brain to the rest of the body.
Intervertebral Discs
Between each vertebra sits an intervertebral disc, which acts like a cushion or shock absorber. Each disc has two main parts:
- Annulus fibrosus: the tough outer layer that provides strength and structure
- Nucleus pulposus: the soft, gel-like center that absorbs pressure and allows flexibility
Bulging Disc vs. Herniated Disc vs. Ruptured Disc
Although these terms are often used interchangeably, they describe different stages of disc damage.
- Bulging disc: The disc extends beyond its normal boundary but the outer layer remains intact. This may or may not cause symptoms.
- Herniated disc: The outer layer weakens or tears, allowing the inner material to push outward and potentially irritate nearby nerves.
- Ruptured disc: A more advanced form of herniation where the inner disc material leaks out, often causing significant nerve inflammation and pain.
Most Commonly Affected Areas of the Spine
Cervical Spine (Neck)
Herniated discs in the cervical spine can cause neck pain along with symptoms that radiate into the shoulders, arms, and hands. Headaches, numbness, and weakness may also occur depending on which nerve is affected.
Lumbar Spine (Lower Back)
The lumbar spine is the most common location for herniated discs due to the amount of weight and stress it supports. Symptoms often include lower back pain that travels into the hips, buttocks, or legs—commonly referred to as sciatica.
Herniated Disc Diagnosis in Kennesaw
Comprehensive Clinical Evaluation
Your evaluation begins with a detailed, face-to-face assessment designed to connect your symptoms with the underlying spinal issue.
Key components of the clinical evaluation include:
- Detailed patient history
- When symptoms began and how they have progressed
- Activities or injuries that may have triggered the pain
- Pain patterns, severity, and what worsens or relieves symptoms
- Prior treatments and how your body responded
- Physical and neurological examination
- Testing reflexes, sensation, and muscle strength
- Identifying signs of nerve irritation or compression
- Comparing left vs. right-sided function
- Functional movement and pain assessment
- Observing posture, walking, bending, and range of motion
- Identifying movements that reproduce or relieve pain
- Evaluating how pain impacts work, sleep, and daily activities
Advanced Diagnostic Imaging
Imaging is used strategically—to confirm findings from your exam and pinpoint the exact source of pain.
Common diagnostic tools include:
- X-rays
- Show spinal alignment, bone structure, and signs of instability or arthritis
- What they cannot show: disc herniations or nerve compression
- MRI (Magnetic Resonance Imaging)
- Considered the gold standard for evaluating herniated discs
- Clearly visualizes discs, nerves, spinal cord, and soft tissues
- Identifies the size, location, and severity of a disc herniation
- When additional testing may be required
- Persistent or complex symptoms
- Prior spine surgery
- Suspected nerve damage or overlapping conditions
- Advanced studies may help refine diagnosis and guide treatment decisions
Accurate Diagnosis = Better Outcomes
Not all back or neck pain comes from a herniated disc—even when imaging shows disc changes. Treating the wrong structure can delay recovery.
Why precision matters:
- Identifying the exact pain generator
- Disc, nerve, joint, muscle, or a combination
- Ensures treatment targets the true source of symptoms
- Avoiding unnecessary procedures or medications
- Prevents overuse of pain meds or injections that won’t help
- Reduces risk of overtreatment or ineffective interventions
- Creating a more effective, personalized treatment plan
- Improves response to conservative and minimally invasive care
- Helps patients recover faster with fewer setbacks
Non-Surgical Herniated Disc Treatment Options
Physical Therapy & Corrective Exercise
Targeted physical therapy is one of the most effective tools for herniated disc recovery when guided by proper diagnosis.
Key goals of therapy include:
- Core stabilization and spinal support
- Strengthening the muscles that support the spine
- Reducing stress on the injured disc during daily movements
- Improving flexibility and posture
- Restoring healthy motion in stiff or guarded areas
- Correcting posture that contributes to ongoing disc strain
- Preventing recurrence
- Teaching safe movement and lifting mechanics
- Building long-term strength to protect the spine after pain improves
Medication Management (Conservative & Non-Addictive)
Medications may be used strategically to help manage pain and inflammation—without relying on long-term or high-risk solutions.
Common approaches include:
- Anti-inflammatory strategies
- Reducing swelling around irritated nerves
- Helping improve comfort so patients can stay active and engaged in therapy
- Muscle relaxants when appropriate
- Used short-term for painful muscle spasms
- Helps decrease tension that can worsen disc-related pain
- Emphasis on minimizing long-term medication dependence
- Avoiding unnecessary opioids whenever possible
- Using medication as a bridge to healing, not a permanent solution
Interventional Spine Treatments
When pain persists despite conservative care, targeted injections may provide relief by addressing inflammation at its source.
Interventional options may include:
- Epidural steroid injections
- Deliver anti-inflammatory medication near irritated spinal nerves
- Often helpful for radiating arm or leg pain
- Selective nerve root blocks
- Target a specific nerve causing symptoms
- Can be both diagnostic and therapeutic
- Facet joint injections
- Address pain coming from spinal joints that may be contributing to symptoms
How injections help:
- Reduce inflammation around nerves
- Decrease pain signals
- Allow patients to participate more fully in rehabilitation and recovery
Regenerative & Advanced Therapies
In select cases, advanced therapies may be considered to support healing and long-term spine health.
These may include:
- Prolotherapy
- Designed to stimulate the body’s natural repair processes
- May help strengthen supportive spinal structures
- Regenerative medicine approaches (when appropriate)
- Used selectively based on diagnosis and patient needs
- Aimed at improving tissue health rather than masking symptoms
- Supporting the body’s natural healing response
- Enhancing recovery while avoiding unnecessary surgical intervention
- Aligning with a least-invasive, function-focused philosophy
Recovery and Rehabilitation After Herniated Disc Treatment
Recovery doesn’t end when treatment is completed—it’s an essential phase of long-term success. Whether care involved conservative therapies, injections, or minimally invasive surgery, guided rehabilitation plays a vital role in restoring strength and preventing recurrence.
Expected recovery timelines (vary by treatment type):
- Non-surgical care: gradual improvement over weeks as inflammation decreases and movement improves
- Injection-based treatments: symptom relief may begin within days to weeks
- Minimally invasive surgery: many patients resume light activity within days, with steady progress over several weeks
Why guided rehabilitation matters:
- Helps restore normal movement patterns safely
- Strengthens muscles that protect the spine
- Reduces the risk of re-injury during the healing process
Lifestyle modifications for long-term spine health include:
- Maintaining a healthy activity level and body weight
- Avoiding prolonged static positions
- Incorporating regular, spine-friendly exercise
Ergonomics, posture, and movement education:
- Proper workstation setup at home and work
- Safe lifting and bending techniques
- Awareness of daily habits that place unnecessary strain on the spine
Preventing future disc injuries:
- Building core strength and flexibility
- Continuing home exercise programs after formal therapy ends
- Addressing minor symptoms early before they become major setbacks
Start Your Path to Relief Today
Living with herniated disc pain can feel overwhelming—but recovery is possible. With the right diagnosis, a thoughtful treatment plan, and expert guidance, many patients are able to regain comfort, movement, and confidence without invasive procedures. There is real hope for improvement, even if your pain has been present for months or years.
If you’re experiencing persistent back or neck pain, radiating symptoms, numbness, or weakness, you don’t have to navigate it alone. Seeking expert guidance early can help you understand your options—without pressure—and choose a path that aligns with your goals and lifestyle.
Contact Medici Orthopaedics & Spine
At Medici Orthopaedics & Spine, care is centered on restoring quality of life using the most effective, least invasive approaches available.
- Website: https://www.mediciortho.com/
- Main Phone: +1-844-328-4624
Kennesaw Clinic
2911 George Busbee Parkway
Suite 50
Kennesaw, GA 30144
(770) 545-6404